“Will it become a productive process putting patients’ choice and empowerment first, or is it all talk, hurling stones at one another, going round in circles and building nothing?”
“Will it become a productive process putting patients’ choice and empowerment first, or is it all talk, hurling stones at one another, going round in circles and building nothing?”
Since The Lords voted to reject proposed amendments last week, to legislation which would have emphasised patient empowerment in the programme and shored up trust, I feel a little in limbo.
As patients of the NHS in recent times, we have been bombarded with the language of patient choice, personalised care and patient empowerment. Putting patients first.
But what power or choice do we patients really have in the use of our health data?
It seems that increasingly media articles, meeting minutes and speeches talk of power and patient empowerment, but it feels like in reality we have less and less.
So too we hear repeated how ‘powerful’ our health data is. How the power of data and its management is used, how the concomitant language is used, misused and shared with others, influences decision making around the subject and our patient rights.
All things are subject to interpretation. Whichever interpretation prevails at a given time is a function of power and not of truth. – Friedrich Nietzsche
As a Germanist at university, interpreting Nietzsche was both a cause for celebration and a cause of much gnashing of teeth. Having also studied Italian, I’m mixing my Dante in there, apologies.
The gnashing of teeth, biblical in origin, was reserved by Dante for the fourth circle of Hell, in his most famous work of his trilogy, the Divine Comedy. The fourth circle was the realm of money. It contained two opposite groups, the avaricious and the squanderers. The bridge builders and the destroyers.
Both the hoarders and the wasters are obsessed with development, either promoting it, or stopping it at all costs. And their punishment is to go round in circles, labouring against each other with heavy rocks, from opposing sides for eternity.
My background is in making technology functional for users to make their work easier. Systems only work which have a proven benefit for the stakeholders. Introducing new systems is not about technology, but about people. If people don’t want to use your system, you can’t make them. They will find a workaround or data quality will be so poor as to make it worthless. Any project with opposing sides, will have some degree of argument and failure for one or more parties. It’s not what working together, should be about.
When I heard the Lords debate, two things struck me.
The first, whilst different arguments were debated they were really not opposed to one another, but trying to find the best way of achieving the project aims. The vast majority were common sensed and aligned. Wellcome and the AMRC support the legislative shoring up of trust. The biggest difference was that citizens’ trust and empowerment were supported better by the amendments, yet the vote went the other way.
The second thing which struck me, was how the language used can sway what we believe. We only believe what we want to believe, after all.
Labelling data as anonymous or de-identified when what is meant is pseudonymous, and mixing in ‘Open Data’ when ‘shared data’, is meant, is not the same thing at all. And it’s very misleading.
The Lords ‘ping pong’ last week again misrepresented, I feel, the weight that anonymous data sharing should have in the debate.
Earl Howe said;
“I stress this point in particular, as I understand that it has been the subject of some confusion. There is already a strong legal framework protecting the confidential and identifiable data held in people’s health and care records, not just the information held by the HSCIC but more generally. The Data Protection Act, which implements the EU data protection directive into UK law, provides powerful protection of information about living individuals. To summarise what is a lengthy and complex provision, it requires all such data to be anonymised except where there is good reason to the contrary. It remains the case that the Data Protection Act continues to offer strong protection of personal data…”
The fact he wants to make such efforts to ‘stress this point in particular’ does not fill me with faith in the system. In fact, I’ll be honest, I feel that on this point he was factually misleading.
Firstly, in terms of extraction.
The default position is to extract fully identifiable and personal data unless individuals object. PCD will leave the practice for all patients, where there is a legal basis i.e. under the HSCA 2012 or Section 251 approval.
So for Earl Howe to focus on anonymous use, detracts from the fact that it is not anonymous upon extraction at all and may be used and is used with identifiers, far more widely than patients might expect once processed. And will be by default, unless people activley opt out.
Misuse and inappropriate levels of risk exposure are made less transparent by the wording of what type of data it is.
Time and time again, even in the Lords last week, I am frustrated to hear inappropriate use of terminology which perpetuates misunderstanding.
We need to be very clear what differences there are between data sharing and Open Data. Professor Sir Nigel Shadbolt addressed these differences and the release of Open Data at this conference on March 20th 2014. He importantly makes the distinction that the reusable open-to-use-by-anyone data of Open Data definition, is separate from most uses of personal data, even in the current ‘grab’ going on. [his words]
The Open Data movement is not trying to liberate and put out all our personal data. He sees personal data, fully and properly anonymised, with consent, will play a role. But we need to understand different ways of handling the different types of data.
Governmental legal guidance in 2010 did not have the interpretation we have been given today of amber, pseudonymous data. In this file you’ll see it’s personal (red) or it’s not (therefore fully anonymous). But it is clearly noted that anything which is not fully anonymous, i.e. what may identify individuals (what HSCIC labels Amber), should be treated no differently from red data.
“If the data to be shared is fully anonymised, then it will be less likely for problems should arise, though consideration still has to be given to the principles in the Data Protection Act 1998 (DPA). If the data required for statistical purposes contains information which may identify individuals (personal data), then the sharing should be approached in the same way as for any other circumstances, as explained in this guidance.”
I have no idea by whom and for whom it was written, but they state they consulted ICO.
We need to be clear, this is important both for public and parliamentary perception to make informed choices and inform the parliamentary care.data and wider data sharing debate.
In Parliament yesterday, Chi Onwurah MP (14 May 2014 : Column 848) said with regard to the Apprenticeships, Skills, Children and Learning Act 2009 – my bold:
It is therefore deeply troubling that the Government have tabled a last-minute new clause to the Bill to authorise data sharing among the Department for Business, Innovation and Skills, Her Majesty’s Revenue and Customs and persons providing services to them when it comes to apprenticeships. This may be both necessary and useful—the actual data to be shared may be entirely harmless—but it should be done transparently, with the right safeguards and accountability in place, and it should be done as part of a coherent strategy. This is clearly not the case here. The “person providing services” could be anyone, from individual consultants to big multinational companies.
We therefore tabled amendment (a) to ask what information was being shared, with whom, by what process, with what accountability, and how it fitted into the Government’s data sharing strategy. If the Minister can answer all those questions, perhaps the amendment will prove superfluous. If not, why not?
Doesn’t it sound rather familiar? Rushed amendment, lack of transparency, loose terminology of data recipients and purposes. If data is presented in wording which is inaccurate, we can only expect its use to be so too.
We need to ask what is the Government’s data sharing strategy and whom does this legislation serve?
Increasingly it seems to me that the Government is firefighting ad hoc bits of data legislation into existing Bills to enable their initiatives which need our personal data. We are being mined on all fronts. Open Data across the board, HMRC plans, DWP, the NPD, DVLA, care.data and more. And mostly, without our consent and often without our informed knowledge.
How is this empowering patients and citizens by removing our choice or rights of autonomy?
Some data sharing programmes may have been addressed and work well. But it takes more than a bathful of corks, to make a watertight boat. It sounds to an outsider, like overall data sharing design and strategy needs to go back to the drawing board and draw up a decent infrastructure. Patching like this, is a waste of time IMO and we can just sit back, and await the future leaks. I just hope they won’t be nightmare stories in health.
All in all, ‘you have a choice’ sounds rather hollow in all manner of fields right now. It’s been a bad week for patient power from where I write. Our local GP practice caring for 4,000 patients is set to close at the end of the month and the list shared out to three already full alternative practices.
Tim Kelsey as Director for Patients and Information outlined in 2012:
“making data available to the public does drive choice in the same way it would in consumer markets such as financial services or mobile telephones or whatever.”
Freed data was seen to walk hand-in-hand with choice. We were told with patient choice, would come patient empowerment. The NHS was turned into a consumer market in the HSC Act 2012.
It’s therefore ironic that the foundations of care.data fail to put patient choice as its cornerstone. It’s not a consent process which is set out by the HSCA 2012 (250-60’ish). It’s a gateway for extraction with no more than fair processing requirement. That loss of autonomy is not giving patients control nor choice. And the choice that is on offer, is limited. Both in scope and time. The only choice offered in the patient leaflet and communications, is to restrict fully identifiable onward data sharing from GPs or from HSCIC. And to be excluded from care.data is a limited offer – before it is launched. After that, the only choice left is to request the data which has been extracted is made pseudonymous, but it is not possible to remove it.
There can be no arguing with what has happened in the past regarding data releases which may no longer be seen as wise. Despite the fact the Information Centre cannot tell us today, (Q272) who all the end users of data have been in the past, we are offered no new barriers to breaches of trust happening again.
The Health and Social Care Act 2012 brought in fundamental changes in both practice and balance of power between patient and provider, and the State. These are changes in society over which we have little control, for now. Come the next General Election, there may be political change and ideology may be different. It may not be. And inevitably in our current political system, it will swing between different thinkings over time. But our health records given up today, are given up for life. Commercial exploitation is a value set being thrust upon us, which we may or may not not embrace. Both in terms of with whom our data is shared, who is managing it and how.
I met my own MP last week, thanked him for sharing my concerns with the Department of Health last October, and discussed the current status of the programme. He asked me, was I against sharing our medical records at all costs? To which my answer was no. No with a number of caveats.
We are used to, what most would see in this country, as a benign government. Events around the world, show us that we should not take it for granted. (I imagine at this point a failed Conservative election 2015, Boris with his cornflake model for society, replaces Cameron at some point in the next term, and wins in 2018 with support of a minority UKIP coalition. My personal result from hell. Don’t forget to vote May 22nd!)
If we have no statutory strength, what do patients really have power over in the choice to share our medical records?
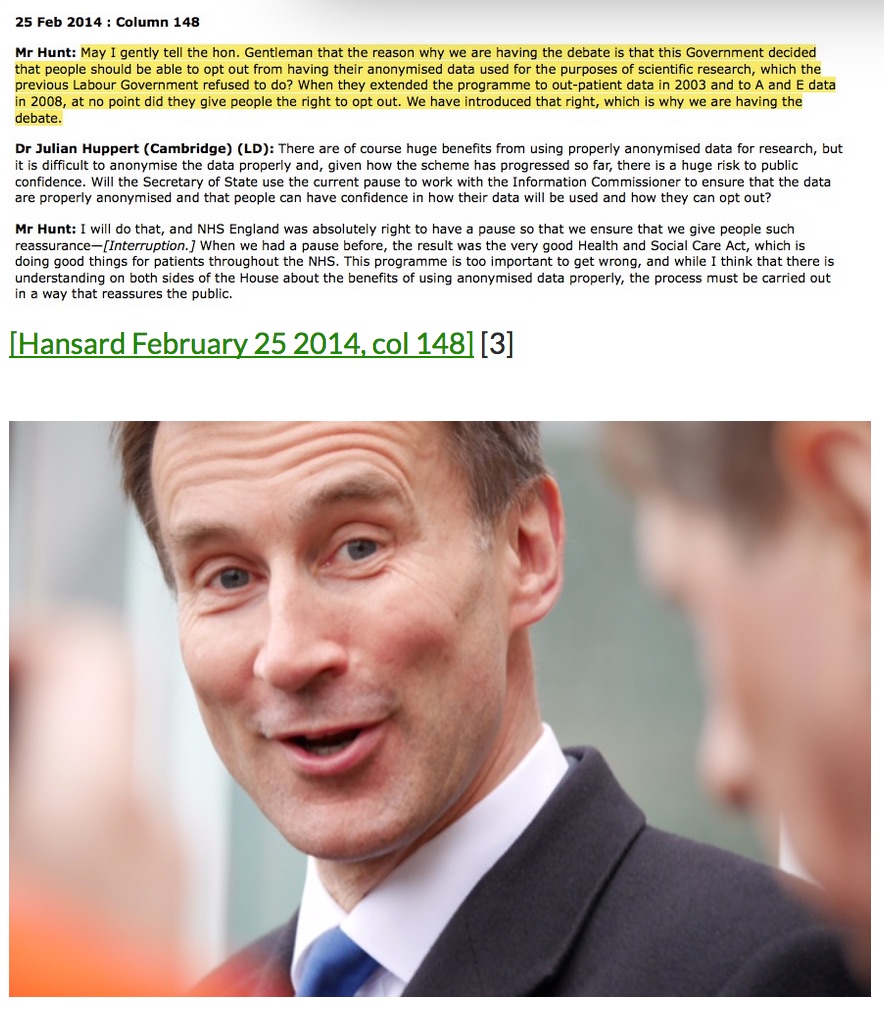
So far we have only an objection to identifiable data sharing. No opt out of other data sharing from HES at all has been offered in patient communications. No opt out form and nothing in law. And Mr.Hunt’s word of ‘an objection which will be respected’ but does not yet match with what he promised on February 25th, and opt out of anonymised data used in research.
…”we said that if we are going to use anonymised data for the benefit of scientific discovery in the NHS, people should have the right to opt out”
That’s not only on identifiable data as the patient leaflet proposed. However I fear this may once again become subject to interpretation. Mr.Hunt has the power to make his promise a reality. I would greatly respect what he says, if we see his words become action.
In 2009 Mr.Kelsey voiced his opinion on opt out, in article published in his name in Prospect.
“no one who uses a public service should be allowed to opt out of sharing their records. Nor can people rely on their record being anonymised..”
So who holds the power to make the decision? Mr.Hunt, Mr.Kelsey or do they mean what they say, they want empowered patients?
Whilst there are individuals who appear obsessed with pushing forward the promotion of health data sharing, at all costs, whether with their own Life Science company background interests, or with a vision of how we will mash it up with supermarket loyalty cards, others may be pushing back, immovably opposed to the whole idea of removal of GP patient confidentiality.
Unlike the fourth circle of Hell, there appears to be a more commonly held middle ground.
However, reality is that the opt out does not work like that yet. So far, we do not have a communicated choice on amber HES.
So even for those who support some data sharing, whilst trust hangs in the balance, people will not support a system which appears to deliberately disempower us. By first starting with opt out, care.data is skewed to removing patient choice from those who are not paying attention to public issues and we’re not sure of the security of the objection on offer anyway. Those who are alert, mainly dislike the idea of our data being traded with third parties who may use the data to create knowledge which they sell on, for profit. When we see stories of who uses it and how, we feel let down.
It feels both an abuse of trust and of power, that having trusted ‘the system’, we have been failed by its gatekeepers and guardians.
It is ironic that in a society in which news and campaigns persistently remind our children that their bodies are their own, that the knowledge of their workings will be taken from them without their knowledge or future ability to withdraw their consent and remove their records. In their lifetime, it might not only be e-data but biomedical.
Within assumed consent and opt out based on an honour system, is the question of power and control. There is one person making a decision who can choose whether or not to respect our objection.
We have only his word, that we have an objection to share any individual identifying data from our GP practice.
The patient leaflet says, ‘you have a choice.’
In reaching our choice, I also ask if we are each individually empowered to make it of our own free will, or will we be emotionally ‘encouraged’ to see it as the right thing to do?
Perhaps made to feel selfish if we do not. Is this free and informed, and not coercion?
Citizens must be pro-active to opt out. The last letter from May 2nd online from Mr.Kelsey suggested we can work together, to get care.data right. However, in the same letter our patient choice, comes at a price. Whilst being encouraged to see reasons to stay opted in and give up our data, we are told of a patient who was misdiagnosed and died.
“In future, this can help prevent cases such as Alison, from Hampshire, who went to her GP suspecting she had a brain tumour, but was prescribed painkillers. She was eventually diagnosed in A&E after a seizure and died less than a year later.”
I feel when I read that, it came across very much as, “see what happens if you don’t share your data? You’ll die prematurely” and the second statement on cancer in A&E made us feel guilt that we may not help us identify why someone else who died. And if fear and guilt are not strong enough sticks, here’s the carrot, by sharing our data we’ll keep it safer somehow, by entrusting it to the State:
“minimise the risk to a person’s privacy being compromised in an age of increasingly sophisticated digital threats.”
(Erm, let me keep it only accessible by my GP practice then, rather than risk sharing it via Google Cloud?)
Please. Stop chivvying us into doing what you want. We have a choice. The leaflet, which we may or may not have ever received, told us so on the front cover. You cannot also tell us what to choose. Big Brother, you don’t have the right to make up our mind for us. No matter your own experiences, whether it’s a family friend’s care, or the terminal illness of a son, or indeed each of our own family experiences. None of us have the right to decide what is a correct decision for others. Neither should Mr. Hunt be asking GPs to ‘sell’ the programme to patients. It’s an abuse of power to coerce a free choice.
I don’t want to feel emotionally manipulated. Just be straight talking and trust us to make up our mind as we see fit.
Overly aggressive charity collector chuggers asking for cash donations on the street, get short shrift these days. It feels like the programme is still trying the same, with mildly threatening tactics in order to use our data, by research charities among others. The lesson why that’s not right seems not to have been learned. The Wellcome Trust clearly does understand what is needed and backed the Lord Howe’s governance and oversight proposal. (Col 1520).
The letter also gave the impression that poor or missed diagnoses in primary care were responsible for disproportionately finding cancer in A&E, which was disputed on social media Twitter by medics suggesting similar use of statistics had been previously corrected, when NHS England retracted it last autumn. Another lesson not learned. Is it an abuse of statistical data if whilst factual, it is knowingly being misunderstood and creating misinformation. One could also ask, is this not an abuse of the power of data and anecdote?
Dante was a tad cheeky in the Comedy. He sought to create his own immortality. By retelling the stories of the damned, he created his own power over them. He controls the narrative, selecting whose stories get shared and those which do not. He is selective with the truth. He believes that by interpreting others’ stories he could give them, and himself, an eternal life. He puts himself among the great poets who have gone before him and enjoys their glory.
He is led through Hell, by Virgil, someone he both adulates and trusts.
So too patients need leadership we can trust and respect. We need transparent and accurate truth, if we are to build trust. There is no room for emotional blackmail.
There should be no power struggle in a free decision. Like in the Divine Comedy, there’s lots of rights and wrongs, differing ethics and moral dilemmas to consider. But judgement should not be made.
Personally I believe it is not right that we parents should determine now what should be our children’s choice, with no correction nor future opt out. Not everyone *is* a willing research patient, and that’s OK. Others may want to be as involved as possible. Only 4% of the population are blood donors, but I’m not going to browbeat anyone into doing it who isn’t.
A stick is still a stick, even if you tell us in your opinion, it’s the right thing to do. You want to empower patients? Prove it. Empower us with statutory opt out and trust us to make our own choice.
Put patients first and show us you mean it.
Will it become a productive process putting patients’ choice and empowerment first, or is it all talk, hurling stones at one another, going round in circles and building nothing?
Does Mr. Hunt, Government and NHS England really want to involve patients about decisions made in the NHS, and in the use of our health data in particular?
What powers-at-be are deciding how our data is managed and governed and who can have it and why?
One of my favourite mottos is found in ‘Inferno’, Dante’s Hell.
“The hottest places in hell are reserved for those who, in a time of moral crisis, maintain their neutrality.”
In Dante’s Commedia, treachery against religion and against government are both reserved for Hell’s final circle.
I hope my public stance is helpful. I fear it has become a bit of a rant. Apathy is neutral. But this is no time for neutrality. There are those in power who make decisions, those with power who influence them and the rest of us. We need to speak up.
To protect our patient choice and to ask to exercise our patient power, so oft championed in word by NHS England and Government, feels so far, rather a risky position to take and challenge what is yet an empty promise. But public opinion should not be ignored when considering what is deemed to be in the Public Interest. We need a more interested public to understand what it will mean if our health data is given freely to third parties, perhaps cross borders, in pseudonymous form without data protection controls or any need to respect consent or inform us. Not just today, but for our lifetime and beyond.
We need some good interpretation and good bridge builders.
We need leaders we can trust to lead us through this process and positively out the other side.
..”every single NHS patient should have a right to opt out of having their data used in anonymised scientific research. I think that was the right thing to do. Of course we are having a difficult debate, but its purpose is to carry the public with us so that we can go on to make important scientific discoveries.”
[Jeremy Hunt, 25th February 2014 – col 148]
Power to the People, was timely this week. Is it all talk, or do you trust us to make our own choices? Trust is a two-way process. You want us to trust the system? Give us a statutory opt out. Get the governance and oversight procedures sorted out. Narrow the commercial purposes for which data can be used.
I think patients can see the benefits of the programme, but it’s going to be hell getting to a workable solution if basic patient empowerment is left off the discussion table. After all, it’s our data.
PS: (The remix of power to the people may be better than the original.) Maybe there’s a second chance for most things.