The Freedom of Information Act has enabled me to stand up for my children’s rights. It really matters to me. And we might lose it.
For every member of the public, who has ever or who has never used their rights under the Freedom of Information Act laws, the government consultation on changing them that closes today is worth caring about. If you haven’t yet had your say, go and take action here >> now. If it is all you have time for before the end of today, you can sign 38 degrees petition or write an email to your MP.
Or by the end of today you can reply to the call for evidence. There is further guidance on the Campaign For Freedom of Information’s website. 38 Degrees have also got this plain English version.
Please do. Now. It closes today, on November 20th.
If you need convinced why it matters to me and it should to you, read on.
What will happen
If the proposed changes come to pass, information about public accountability will be lost. Political engagement will not be open to all equally. It will promote an unfair society in which individuals are not only prevented from taking part in full public life, but prevented from understanding decisions made about them or that affect them. Campaign groups will be constrained from standing up for human rights by cost. The press will be restrained in what they can ask.
MySociety has a brilliant summary. Michael Sheen spoke up calling it “nothing short of a full frontal attack” on the principles of democratic government. And Tom Watson spoke of three serious instances where facts would have stayed hidden, were it not for access made using the law of Freedom of Information:
1. death rates in cardiac patient care
2. cases when the police use Tasers on children
3. the existence of cracks in the nuclear power station at Hinckley
Why does FOI matter to me personally? In Education.
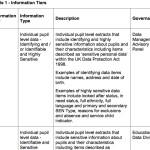
Because it’s enabled me to start a conversation to get the Department for Education to start to improve their handling of our 8 million children’s personal and sensitive data they hold in the National Pupil Database for England and Wales. Through FOI I asked for unpublished facts how many releases of identifiable personal data of school pupils have been fast-tracked at the Department of Education without panel oversight. And to see the panel terms of reference which are still not on their website.
The request: whatdotheykknow.com
The outcome: National Pupil Database FOI case study summary here.
I’m now coordinating calls for changes on behalf of the 8m children whose records they hold and parents across the country.
******
Why does FOI matter to me personally? In Health.
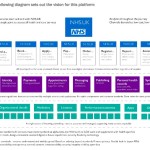
Because Freedom of Information law has enabled public transparency of decision making and accountability of the care.data programme board decision making that was kept secret for over a year. NHS England refused to publish them. Their internal review declined appeal. The Information Commissioner’s Office upheld it.
The current protection afforded to the internal deliberations of public bodies are sufficient given section 35 and 36 exemptions. In fact my case study, while highlighting that NHS England refused to release information, also shows that only a handful of genuine redactions were necessary, using Section 36 to keep them hidden, when the minutes were finally released.
In October 2014 I simply wanted to see the meeting minutes form part of the public record of care.data planning. I wanted to see the cost-benefit business case and scrutinise it against the benefits case that the public were told of at every public engagement event I had been to. When at every turn the public is told how little money the NHS can afford to spend I wanted scrutiny of what the programme would cost at national and local levels. It was in the public interest to better inform public debate about the merits of the national programme. And I strongly believe that it is in the public interest to be informed and fully understand the intention and programme that demands the use of sensitive personal data.
The request: whatdotheyknow.com
The outcome: care.data FOI case study summary here.
Others could use this information I hoped, to ask the right questions about missing meeting minutes and transparency, and for everyone to question why there was no cost-benefit business plan at all in private; while the public kept being told of the benefits. And it shows that data collection is further set to expand, without public debate.
Since then the programme has been postoned again and work is in progress on improved public engagement to enable public and professional confidence.
What has Freedom of Information achieved?
One of the most memorable results of Freedom of Information was the MPs expenses scandal. Who knows how much this Freedom of Information Request saved the taxpayers in immeasurable amounts of future spending on duck houses since MPs have been required to publish expenses since 2010? Four MPs were jailed for false accounting. Peers were expelled. Second homes and what appeared to the public as silly spending on sundries were revealed. Mr. Cameron apologized in 2009, saying he was “appalled” by the expenses. The majority of MPs had done nothing illegal but the Freedom of Information request enabled the start of a process of increased transparency to the public which showed where activities, while permitted by law, were simply unethical or unreasonable.
Historical record
Information published under the Freedom of Information Act can help to ensure that important records of decision-making processes are retained as part of the historic background to government.
Increased trust
The right information at the right time helps make better decisions, make spending more transparent and makes policies and practices more trustworthy.
Access to official information can also improve public confidence where public sector bodies are seen as being open. In a 2011 survey carried out on behalf of the Information Commissioner’s Office, 81% of public bodies questioned agreed that the Act had increased the public’s trust in their organisation.
A key argument made by the commission is that those in public office need private space for decision making. The Information Commissioner’s Office countered this in their submission to the consultation saying,
“there is a distinction between a need for a private space, depending on the circumstances and a desire for secrecy across a broad area of public sector activity. It was the latter tendency that FOIA was intended to correct.”
So how much more “private space” do public servants need?
Holding back information
When information that are judged should not be released in the public interest, there are already exemptions that can be applied to prevent disclosure of information under the Freedom of Information Act. [1]
The exemptions include:
- if the information can easily be accessed by other means – e.g. the internet or published documents
- if the information is personal information
- if the information is provided in confidence (but only if legally enforceable)
- when there is a legal reason not to disclose
- if the information is about national security, defence, the economy, law enforcement, formulation of Government policy, health and safety, communications with Her Majesty or other royalty, international relations, intended for future publication and commercial interests. (All exemptions in this group must be tested to see if disclosure is in the public interest.)
In addition to these exemptions, organisations can withhold information if it will take more than two-and-a-half days to provide it, or they cannot identify what information is needed (although they have to work with the requester to clarify what is being requested).
They can also withhold information if they decide the request is vexatious.
Does it cost us too much to administer?
Some people who are supportive of these changes say they are concerned about costs in answering requests but have perhaps not considered the savings in exceptional cases (like the Expenses Scandal outcome). And as mySociety has reported [2], money spent responding to Freedom of Information requests also needs to be considered fairly in the context of wider public spending. In 2012 it was reported that Staffordshire County Council had spent £38,000 in a year responding to Freedom of Information requests. The then Director of mySociety, Tom Steinberg, commented:
“From this I can see that oversight by citizens and journalists cost only £38,000 from a yearly total budget of £1.3bn. I think it is fantastic that Staffordshire County Council can provide such information for only 0.002 per cent of its operating budget.”
Why does the government want to make itself less transparent? Even the Information Commissioner’s office has replied to the consultation to say that the Commissioner does not consider that significant changes to the core principles of the legislation are needed. This is a good law, that gives the public rights in our favour and transparency into how we are governed and tax money spent.
How will the value of FOI be measured of what would be lost if the changes are made?
What can you do?
The call for evidence is here and there is further guidance on the Campaign For Freedom of Information’s website. 38 Degrees have also put together this super-easy Plain English version.
To have your say in the consultation closing on November 20th go online.
Or simply call or write to your MP. Today. This really matters.
References:
[1] Requests can be refused https://ico.org.uk/for-organisations/guide-to-freedom-of-information/refusing-a-request/
[2] MySociety opposes restrictions https://www.mysociety.org/2015/11/11/voices-from-whatdotheyknow-why-we-oppose-foi-act-restrictions/
[3] National Pupil Database FOI case study summary here
[4] My care.data programme board FOI case study summary here


![Building Public Trust in care.data datasharing [3]: three steps to begin to build trust](https://jenpersson.com/wp-content/uploads/2015/06/optout_ppt-672x372.jpg)
![Building Public Trust in care.data sharing [1]: Seven step summary to a new approach](https://jenpersson.com/wp-content/uploads/2015/07/edison1-672x372.jpg)