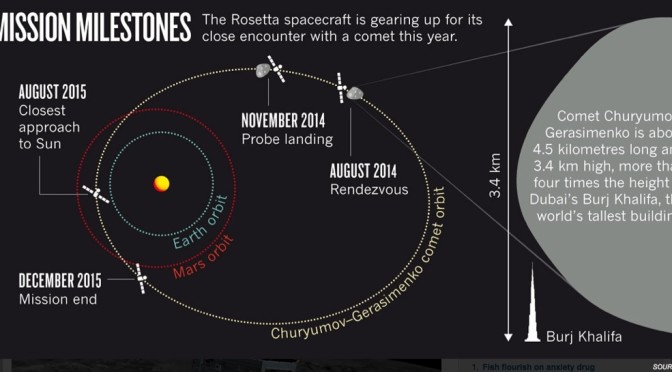
“On Friday 1st August the media reported the next giant leap in the genomics programme in England, suggesting the 100K Genomics Project news was akin to Kennedy launching the Space Race. [1] [from 2:46.30].”
Part two:
What is the expectation beyond 2017?
The investment to date may seem vast if, like me, you are unfamiliar with the amounts of money that are spent in research [in 2011 an £800M announcement, last summer £90M in Oxford as just two examples], and Friday revealed yet more money, a new £300M research package. It is complex how it all adds up, and from mixed sourcing. But the stated aim of the investment is relatively simple: the whole genomes of 75,000 people [40K patients and 35K healthy relatives] are to be mapped by 2017.
Where the boundary lies between participation for clinical care and for research is less clear in the media presentation. If indeed participants’ results will be fed back into their NHS care pathway, then both aims seem to be the intent of the current wave of participants.
It remains therefore perhaps unclear, how this new offering interacts with the existing NHS genetic services for direct clinical care, or the other research projects such as the UK Biobank for example, particularly when aims appear to overlap:.
“The ultimate aim is to make genomic testing a routine part of clinical practice – but only if patients and clinicians want it.” [Genomics England, how we work]
The infrastructure of equipment is enormous to have these sequences running 24/7 as was indicated in media TV coverage. I’m no maths whizz, but it appears to me they’re building Titantic at Genomics England and the numbers of actual people planned to take part (75K) would fit on the lifeboats. So with what, from whom, are they expecting to fill the sequencing labs after 2017? At Genomics England events it has been stated that the infrastructure will then be embedded in the NHS. How is unclear, if commercial funding has been used to establish it. But at its most basic, there will be no point building the infrastructure and finding no volunteers want to take part. You don’t build the ship and sail without passengers. What happens, if the English don’t volunteer in the desired numbers?
What research has been done to demonstrate the need or want for this new WGS project going forwards at scale, compared with a) present direct care or b) existing research facilities?
I cannot help but think of the line in the film, Field of Dreams. If you build it they will come. So who will come to be tested? Who will come to exploit the research uses for public good? Who will come in vast numbers in our aging population to exploit the resulting knowledge for their personal benefit vs companies who seek commercial profit? How will the commercial and charity investors, make it worth their while? Is the cost/benefit to society worth it?
All the various investors in addition to the taxpayer; Wellcome Trust, the MRC, Illumina, and others, will want to guarantee they are not left with an empty shell. There is huge existing and promised investment. Wellcome for example, has already “invested more than £1 billion in genomic research and has agreed to spend £27 million on a world class sequencing hub at its Genome Campus near Cambridge. This will house Genomics England’s operations alongside those of the internationally respected Sanger Institute.”
Whilst the commercial exploitation by third parties is explicit, there may also be another possibility to consider: would the Government want:
a) some cost participation by the participants? and
b) will want to sell the incidental findings’ results to the participants?
[ref: http://www.phgfoundation.org/file/10363 ref. #13]
“Regier et al. 345 have estimated the willingness-to-pay (WTP) for a diagnostic test to find the genetic cause of idiopathic developmental disability from families with an affected child. They used a discrete choice experiment to obtain WTP values and found that these families were willing to pay CDN$1118 (95% CI CDN$498-1788) for the expected benefit of twice as many diagnoses using aCGH and a reduction in waiting time of 1 week when compared to conventional cytogenetic analysis.”“Moreover, it is advisable to minimise incidental findings where possible; health care professionals should not have an obligation to feedback findings that do not relate to the clinical question, except in cases where they are unavoidably discovered and have high predictive value. It follows that the NHS does not have an obligation to provide patients with their raw genome sequence data for further analysis outside of the NHS. We make no judgement here about whether the individual should be able to purchase and analyse their genome sequence independently; however, if this course of action is pursued, the NHS should provide follow-up advice and care only when additional findings are considered to be of significant clinical relevance in that individual…” [13]
How much is that cost, per person to be mapped? What is the expected return on the investment?
What are the questions which are not being asked of this huge state investment, particularly at a time when we are told he NHS is in such financial dire straits?
Are we measuring the costs and benefits?
Patient and medical staff support is fundamental to the programme, not an optional extra. It should not be forgotten that the NHS is a National Service owned by all of us. We should know how it runs. We should know what is spends. Ultimately, it is we who pay for it.
So let’s see on paper, what are the actual costs vs benefits? Where is the overall and long term cost benefit business case covering the multi-year investment, both of tangible and intangible benefits? In my personal research, I’m yet to find one. There is however, some discussion in this document:
“The problem for NGS is that very little ‘real’ information is available on the actual costs for NGS from the NHS perspective and the NHS Department of Health Reference Costs Database and PSSRU, where standard NHS costings are listed, are generally not helpful.” [13 – PHG, 2011]
Where are the questions being asked if this is really what we should be doing for the public good and for the future of the NHS?
Research under good ethics and bona fide transparent purposes is a public asset. This rollout, has potential to become a liability.
To me, yet again it seems, politics has the potential to wreck serious research aims and the public good.
Perhaps more importantly, the unrestrained media hype carries the very real risk of creating unfounded hope for an immediate diagnosis or treatment, for vulnerable individuals and families who in reality will see no personal benefit. This is not to undermine what may be possible in future. It is simply a plea to rein in hype to reality.
Politicians and civil servants in NHS England appear to use both research and the notion of the broad ‘public good’, broadly in speeches to appear to be doing ‘the right thing to do’, but without measurable substance. Without a clear cost-benefit analysis, I admit, I am skeptical. I would like to see more information in the public domain.
Has the documentation of the balance of patient/public good and expected “major contribution to make to wealth creation and economic growth in this country” been examined?
Is society prepared for this?
I question whether the propositions of the initiative have been grasped by Parliament and society as a whole, although I understand this is not a ‘new’ subject as such. This execution however, does appear at least, massive in its practical implications, not least for GPs if it is to become so mainstream, as quickly as plans predict. It raises a huge number of ethical questions. Not least of which will be around incidental findings, as the Radio 4 interview raised.
The first I have is consideration of pre-natal testing plans:
“Aside from WGS of individuals, other applications using NGS could potentially be more successful in the DTC market. For example, the use of NGS for non-invasive prenatal testing would doubtless be very popular if it became available DTC prior to being offered by the NHS, particularly for relatively common conditions such as Down syndrome…” [
and then the whole question of consent, particularly from children:
“…it may be almost impossible to mitigate the risk that individuals may have their genome sequenced without their consent. Some genome scan companies (e.g. 23andMe) have argued that the risks of covert testing are reduced by their sample collection method, which requires 2ml of saliva; in addition, individuals are asked to sign to confirm that the sample belongs to them (or that they have gained consent from the individual to whom it belongs). However, neither of these methods will have any effect on the possibility of sequencing DNA from children, which is a particularly contentious issue within DTC genomics.” [13]
“two issues have emerged as being particularly pressing: first is the paradox that individuals cannot be asked to consent to the discovery of risks the importance of which is impossible to assess. Thus from a legal perspective, there is no ‘meeting of minds’ and contractually the contract between researcher and participant might be void. It is also unclear whether informed consent is sufficient to deal with the feedback of incidental findings which are not pertinent to the initial research or clinical question but that may have either clinical or personal significance…” [PHG page 94]
“What we don’t want to say is those 10 years you have between 70 and 80, although clearly you are not going to be working, are not going to be valuable to somebody.
Clearly they are. You might be doing all sorts of very useful things for your family or local society. That’s what we are worried about and that’s the problem with the Department of Health’s calculation.
There are lots of people who adopt the fair-innings approach; ‘you’ve had 70 years of life you’ve got to accept that society is going to bias its investments in younger people.”
[14 – see Channel 4] Yet our population is ageing and we need to find a balance of where roles, rules and expectations meet. And question, how do we measure human value, should we, and on what basis are we making cost-based care decisions?
The Department of Health proposed that a patient’s economic value should be taken into account when deciding on healthcare. What is their thinking on genomics for the care of the elderly?
Clinical environment changes make engagement and understanding harder to achieve
All this, is sitting on shifting, fundamental questions on how decision making and accountability will be set, in a world of ever fragmenting NHS structure:
“More problematic will be the use of specific genomic technologies such as NGS in patient pathways for inherited disorders that are delivered outside the clinical genetics services (such as services for FH, haemophilia and sickle cell disease) and NGS that is used for non-inherited disease conditions. These will be commissioned by GP consortia within established care pathways. Such commissioning of companion diagnostics would, in theory be evaluated first by NICE. However, it is not clear what capacity NICE will have across a broad range of uses. In practice it seems likely that GP consortia may make a variety of different decisions influenced by local experts and pressure, funding and different priorities. Particular questions for NGS will include: How will commissioners be provided with the necessary evidence for decision-making and can this be developed and coordinated at a national level? How will commissioners prioritise particularly when it may be necessary to invest early in order to achieve savings later? What (if any) influence may commissioners be able to exert over the configuration of test providers (for example the rationalisation of laboratories or the use of private testing companies)? [13]
Is genomics really the lifeboat to which the NHS is inextricably bound?
The Patients and Information Directorate nor wider NHS England Board does not discuss these questions in public. At the July 3rd 2014 Board Meeting, in the discussion of the genomics programme I understood the discussion as starting to address the inevitable future loss of equity of access because of genomic stratification, dividing the population into risk pool classifications [10.42] . To my mind, that is the end of the free-to-all NHS as we know it. And IF it is so, through planned policy. More people paying for their own care under ‘personalisation; is in line with ISCG expectations set out earlier in 2014: “there will be increasing numbers of people funding their own care and caring for others.”
Not everyone may have understood it that way, but if not, I’d like to know what was meant.
I would like to understand what is meant when Genomics England spokespeople say the future holds:
“Increasingly to select most appropriate treatment strategy. In the longer term, potential shift to prevention based on risk-based information.”or“Review the role of sequencing in antenatal and adult screening.”
I would welcome the opportunity to fully understand what was suggested at that Board meeting as a result of our shared risk pool, and readers should view it and make up their own mind. Even better, a frank public and/or press board meeting with Q&A could be rewarding.
The ethical questions that are thrown up by this seem yet to have little public media attention.
Not least, incidental findings: if by sequencing someone’s DNA, you establish there is something for their health that they ought to be doing soon, will you go to that patient and say look, you should be doing this…. these are incidental findings, and may be quite unexpected and separate from the original illness under investigation in say, a family member, and may also only suggest risk indicators, not clear facts.
If this is expected to be mainstream by 2018, what training plans are in place as indicated needed as a “requirement for professionals across the NHS to be trained in genetics and its implications”? [presentation by Mark Bale, DoH, July 2014]
When will we get answers to these questions, and more?
Because there is so much people like me don’t know, but should, if this is our future NHS under such fundamental change as is hyped.
Because even the most esteemed in our land can get things wrong. One of them at the St.Bart’s events quotes on of my favourite myths attributed wrongly to Goethe. It cannot be attributed to him, that he said, ” “Whatever you can do or dream you can, begin it. Boldness has genius, power and magic in it.” You see, we just hear something which sounds plausible, from someone who seems to know what they are talking about. It isn’t always right.
Because patients of rare disease in search of clinical care answers should be entitled to have expectations set appropriately, and participants in research know to what they, and possibly family members indirectly, are committed.
Because if the NHS belongs to all of us, we should be able to ask questions and expect answers about its planning, how we choose to spend its budget and how it will look in future.
These are all questions we should be asking as society
Fundamentally, in what kind of society will my children grow up?
With the questions of pre-natal intervention, how will we shape our attitudes towards our disabled and those who are sick, or vulnerable or elderly? Are we moving towards the research vision Mr.Hunt, Cameron and Freeman appear to share, only for good, or are we indeed to look further head to a Gattacan vision of perfection?
As we become the first country in the world to permit so called ‘three parent children’ how far will we go down the path of ‘fixing’ pre-natal genetic changes, here or in PGD?
How may this look in a society where ‘some cornflakes get to the top‘ and genetic advantage seen as a natural right over those without that ability? In a state where genetics could be considered as part of education planning? [16]
For those with lifelong conditions, how may genetic screening affect their life insurance when the Moratorium expires* in 2017 (*any shift in date TBC pending discussion) ? How will it affect their health care, if the NHS England Board sees a potential effect on equity of access? How will it affect those of us who choose not to have screening – will we be penalised for that?
And whilst risk factors may include genomic factors, lifestyle factors some argue are even more important, but these change over time. How would those, who may have had past genetic screening be affected in future requirements?
After the August 1st announcement, [11] The Wellcome Trust‘s reporting was much more balanced and sensible than the political championing had been. It grasps the challenges ahead:
“Genomics England has ambitious plans to sequence 100,000 genomes from 75,000 people, some of whom will also have cancer cells sequenced. The sheer scale of the plans is pretty daunting. The genetic information arising from this project will be immense and a huge challenge for computational analysis as well as clinical interpretation. It will also raise a number of issues regarding privacy of patient data. Ensuring that these genetic data can be used maximally for patient benefit whilst protecting the rights of the individual participant must be at the heart of this project.
At the beginning of the Human Genome Project, scientists and funders like the Wellcome Trust knew they were on a journey that would be fraught with difficulties and challenges, but the long-term vision was clear. And so it is with the plans for Genomics England, it will most certainly not be easy…”
Managing change
Reality is that yet again, Change Management and Communications have been relegated to the bottom of the boarding priorities list.
This is not only a research technology or health programme. Bigger than all of that is the change it may bring. Not only in NHS practice, should the everyday vision of black boxes in GP surgeries become reality, but for the whole of society. For the shape of society, in age and diversity. Indeed if we are to be world leaders, we have potential to start to sling the world on a dangerous orbit if the edges of scope are ill defined. Discussing only with interested parties, those who have specific personal or business interests in genomic research and data sharing, whilst at Board meetings not clearly discussing the potential effects of risk stratification and personalisation on a free at the point of delivery health service is in my opinion, not transparent, and requires more public discussion.
After all, there are patients who are desperate for answers, who are part of the NHS and need our fair treatment and equity of access for rare disease. There is the majority who may not have those needs but knows someone who does. And we all fund and support the structure and staff in our world class service, we know and love. We want this to work well.
Future research participation depends on current experience and expectations. It is the latter I fear are being currently mishandled in public and the media.
Less than a month ago, at the NHS England Board Meeting on July 3rd, Lord Adebowale very sensibly asked, “how do we lead people from where we are, and how we take the public with us? We need to be a world leader in engaging all the public”
Engagement is not rocket science. But don’t forget the ethics.
If this project is meant to be, according to MP George Freeman [George 2], akin to Kennedy launching the Space Race, then, by Fenyman [12], why can they not get their public involvement at big launches sorted out?
Is it because there are such large gaps and unknowns that questioning will not stand up to scrutiny? Is it because suggesting a programme will end the NHS as we know it, would be fatal for any politician or party who supports that programme in the coming year? Or do the leading organisations possibly paternalistically believe the public is too dim or uninterested or simply working to make ends meet to care [perhaps part of the 42% of the population who expected to struggle as a result of universal welfare changes, one in three main claimants (34 per cent) said in 2012 they ‘run out of money before the end of the week/month always or most of the time’] ? But why bother will the big press splash, if it should not make waves?
In the words of Richard Feynman after the Challenger launch disaster in 1986:
“Let us make recommendations to ensure that NASA officials deal in a world of reality in understanding technological weaknesses and imperfections well enough to be actively trying to eliminate them. They must live in reality in comparing the costs and utility of the Shuttle to other methods of entering space. And they must be realistic in making contracts, in estimating costs, and the difficulty of the projects.
Only realistic flight schedules should be proposed, schedules that have a reasonable chance of being met.
If in this way the government would not support them, then so be it. NASA owes it to the citizens from whom it asks support to be frank, honest, and informative, so that these citizens can make the wisest decisions for the use of their limited resources. For a successful technology, reality must take precedence over public relations… [June 6th 1986. Six months after the disaster, the Report to the Presidential Commission (Appendix F)]
Just like the Rosetta spacecraft is getting ever closer to actually landing on the comet, its goal, [15 – BBC Newsround has an excellent little summary] after over ten years, so too is genomics close to the goal of many. It is within grasp that the long-planned mainstreaming of genomic intervention, will touch down in the NHS. My hope is that in its ever closer passes, we get hard factual evidence and understand exactly where we have come from, and where we intend going. What will who do with the information once collected?
The key is not the landing, it’s understanding why we launched in the first place.
Space may not be the most significant final frontier out there in the coming months that we should be looking at up close. Both in health and science. Our focus in England must surely be to examine these plans with a microscope, and ask what frontiers have we reached in genomics, health data sharing and ethics in the NHS?
****** image source: ESA via Nature
[1] “It’s a hugely ambitious project, it’s on a par with the space race how Kennedy launched 40 years ago.” [from 2:46.30 BBC Radio 4 Int. Sarah Montague w/ George Freeman]
[2] Downing Street Press Release 1st August – genomics https://www.gov.uk/government/news/human-genome-uk-to-become-world-numb
[3] 6th December “Transcript of a speech given by Prime Minister at the FT Global Pharmaceutical and Biotechnology Conference” [https://www.gov.uk/government/speeches/pm-speech-on-life-sciences-and-opening-up-the-nhs]
[4] 10th December 2012 DNA Database concerns Channel 4 http://www.channel4.com/news/dna-cancer-database-plan-prompts-major-concerns
[5] Wellcome Trust- comment by Jeremy Farrar http://news.sky.com/story/1311189/pm-hails-300m-project-to-unlock-power-of-dna
[6] Strategic Priorities in Rare Diseases June 2013 http://www.genomicsengland.co.uk/wp-content/uploads/2013/06/GenomicsEngland_ScienceWorkingGroup_App2rarediseases.pdf
[7] NHS England Board paper presentation July 2013 http://www.england.nhs.uk/wp-content/uploads/2013/07/180713-item16.pdf
[8] ICO and HSCIC on anonymous and pseudonymous data in Computing Magazine http://www.computing.co.uk/ctg/news/2337679/ico-says-anonymous-data-not-covered-by-data-protection-act-until-its-de-anonymised
[9] HSCIC Pseudonymisation Review August 2014 http://www.hscic.gov.uk/article/4896/Data-pseudonymisation-review
[10] November 2013 ISCG – political pressure on genomics schedule http://www.england.nhs.uk/iscg/wp-content/uploads/sites/4/2014/01/ISCG-Paper-Ref-ISCG-009-001-ISCG-Meeting-Minutes-and-Actions-26-November-2013-v1.1.pdf
[11] Wellcome Trust August 1st 2014 The Genetic Building Blocks of Future Healthcare
[12] Fenyan – For successful technology reality must take precedence over PR https://jenpersson.com/successful-technology-reality-precedence-public-relations/
[13] Next Steps in the Sequence – the implications for whole genome sequencing in the UK – PHG Foundation, funded by the PHG Foundation, with additional financial support from Illumina. The second expert workshop for the project was supported by the University of Cambridge Centre for Science and Policy (CSaP) and the Wellcome Trust http://www.phgfoundation.org/file/10363
[14] Anti-elderly drugs proposals rejected by NICE: Channel 4 http://www.channel4.com/news/nice-assessment-elderly-health-drugs-rejected-contribution
[15] BBC Newsround: Rosetta spacecraft and the comet chasing
[16] Education committee, December 4th 2013 including Prof. Plomin From 11.09:30 education and social planning http://www.parliamentlive.tv/Main/Player.aspx?meetingId=14379
*****
For avoidance of confusion [especially for foreign readership and considering one position is so new], there are two different Ministers mentioned here, both called George:
One. George Osborne [George 1] MP for Tatton, Cheshire and the Chancellor
Two. George Freeman [George 2] MP – The UK’s first-ever Minister for Life Sciences, appointed to this role July 15th 2014 [https://www.gov.uk/government/ministers/parliamentary-under-secretary-of-state–42]
*****